Lymphatic Drainage After Joint Replacement: How It Promotes Healing and Recovery
Why lymphatic drainage is essential after hip and knee replacements

Replacing a knee or hip joint is a complex medical procedure that gives many people freedom of movement and quality of life again. But the phase after the operation determines how quickly and successfully a patient recovers. An often underestimated but crucial factor is manual lymphatic drainage (MLD). This procedure promotes the removal of lymph fluid, reduces postoperative swelling and significantly accelerates healing.
In this blog we explain why lymphatic drainage is essential, especially after the insertion of a hip or knee prosthesis, how it works and what advantages it offers.
Basics of lymphatic drainage
What is manual lymphatic drainage?
Manual lymphatic drainage (MLD) is a gentle massage technique specifically aimed at stimulating the drainage of lymphatic fluid in the body. It is mainly used for swelling caused by impaired lymph flow. The lymphatic system is activated by circular, rhythmic movements of the hands.
How does the lymphatic system work?
The lymphatic system is an essential part of our immune system. It transports lymphatic fluid, which contains waste products, proteins and excess tissue fluid, back into the bloodstream. After a surgical procedure such as the insertion of an endoprosthesis, this system can be overloaded.
Joint replacement and the lymphatic system
What role does the lymphatic system play after surgery?
Any surgery, especially on the knee or hip joint, leads to injury to the surrounding tissue. This injury causes an inflammatory reaction that is accompanied by swelling and increased fluid in the affected area. This is where lymphatic drainage comes into play by promoting the drainage of fluid and supporting healing.
Why does swelling occur after joint replacement surgery?
- Traumatic irritation of tissue during surgery.
- Accumulation of inflammatory proteins in the affected area.
- Temporary restriction of lymph flow due to scarring.
Benefits of Lymphatic Drainage After Joint Replacement
1. Swelling reduction
Postoperative swelling is not only uncomfortable, but can also limit mobility. Lymphatic drainage effectively drains excess tissue fluid.
2. Pain relief
By reducing the swelling, pain-causing pressure on surrounding tissue is reduced.
3. Improve mobility
Reducing edema increases joint mobility and makes physiotherapeutic exercises easier.
4. Faster healing
Better blood circulation and reduced inflammation promote cell regeneration and thus healing.
Application of lymphatic drainage after hip and knee prosthesis
When should lymphatic drainage be started?
Lymphatic drainage is usually started just a few days after the operation. The treating doctor and physiotherapist decide together on the right time.
How does a meeting work?
- Duration: 20 to 45 minutes.
- Technique: Gentle, circular movements along the affected lymphatics. This promotes fluid flow towards the central lymph nodes.
- Focus: The focus is on the operated area and the adjacent regions.
How often should lymphatic drainage be done?
In the first few weeks, therapy is recommended two to three times a week. The frequency can be adjusted depending on the healing process.
The effect of lymphatic drainage in detail
Mechanical decongestion
By specifically stimulating the lymph flow, the excess fluid is efficiently removed, which means that swelling subsides more quickly.
Immune system support
Activating the lymphatic system contributes to the faster elimination of inflammatory proteins and supports the immune system.
Improving blood circulation
Lower pressure in the tissue facilitates blood circulation, allowing oxygen and nutrients to be transported better.
Study situation on lymphatic drainage during joint replacement
Scientific evidence
- Studies show that lymphatic drainage can reduce postoperative swelling up to 50% faster.
- Patients report a significant improvement in quality of life.
Clinical success stories
Rehabilitation facilities that rely on lymphatic drainage experience faster recovery and lower rates of complications.
How lymphatic drainage promotes healing after a knee replacement
After knee prosthesis surgery, many patients suffer from swelling in the knee and lower leg area. These edematous processes are a normal consequence of surgery, but without targeted treatments they can slow healing and cause pain. This is where lymphatic drainage comes in – a form of therapy that specifically aims to reduce edema and thus positively influences the healing process.
Physiological effect of knee prosthesis
Lymphatic drainage increases the reabsorption of tissue fluid by activating the lymphatic vessels. This reduces the pressure in the tissue, which in turn promotes blood circulation and accelerates wound healing. The decongestion has a direct effect on:
- Pain relief because the pressure on nerve endings decreases.
- Improved mobility as swelling restricts joint movement.
- Reduction in the risk of infection because there is less stagnant fluid in the tissue.
Psychological benefits of lymphatic drainage
In addition to the physical effects, lymphatic drainage also offers psychological relief. Patients often feel calmed and more relaxed as a result of the direct, gentle treatment, which in turn promotes healing. This mental component is often underestimated, but is an essential factor in the rehabilitation process.
How lymphatic drainage promotes recovery after hip replacement
Even after hip replacement surgery, lymphatic drainage is one of the most effective methods to minimize swelling and postoperative discomfort.
Typical challenges after hip replacements
Swelling in the groin, thigh or area of the surgical field makes mobilization difficult and puts strain on the surrounding tissue. Tense muscles due to the surgical manipulation and difficult lymph flow can hinder healing.
How does lymphatic drainage help with hip replacement?
- Activation of lymphatic flow: Therapists use gentle pressure to direct the accumulated tissue fluid into the functioning lymphatics.
- Lowering Inflammation Levels: Decongestion reduces pain caused by inflammation.
- Supporting mobilization: Relieved tissue feels more mobile, making early mobilization easier.
Special considerations for hip replacements
- The lymphatic drainage pathway must be carefully directed around the operated region.
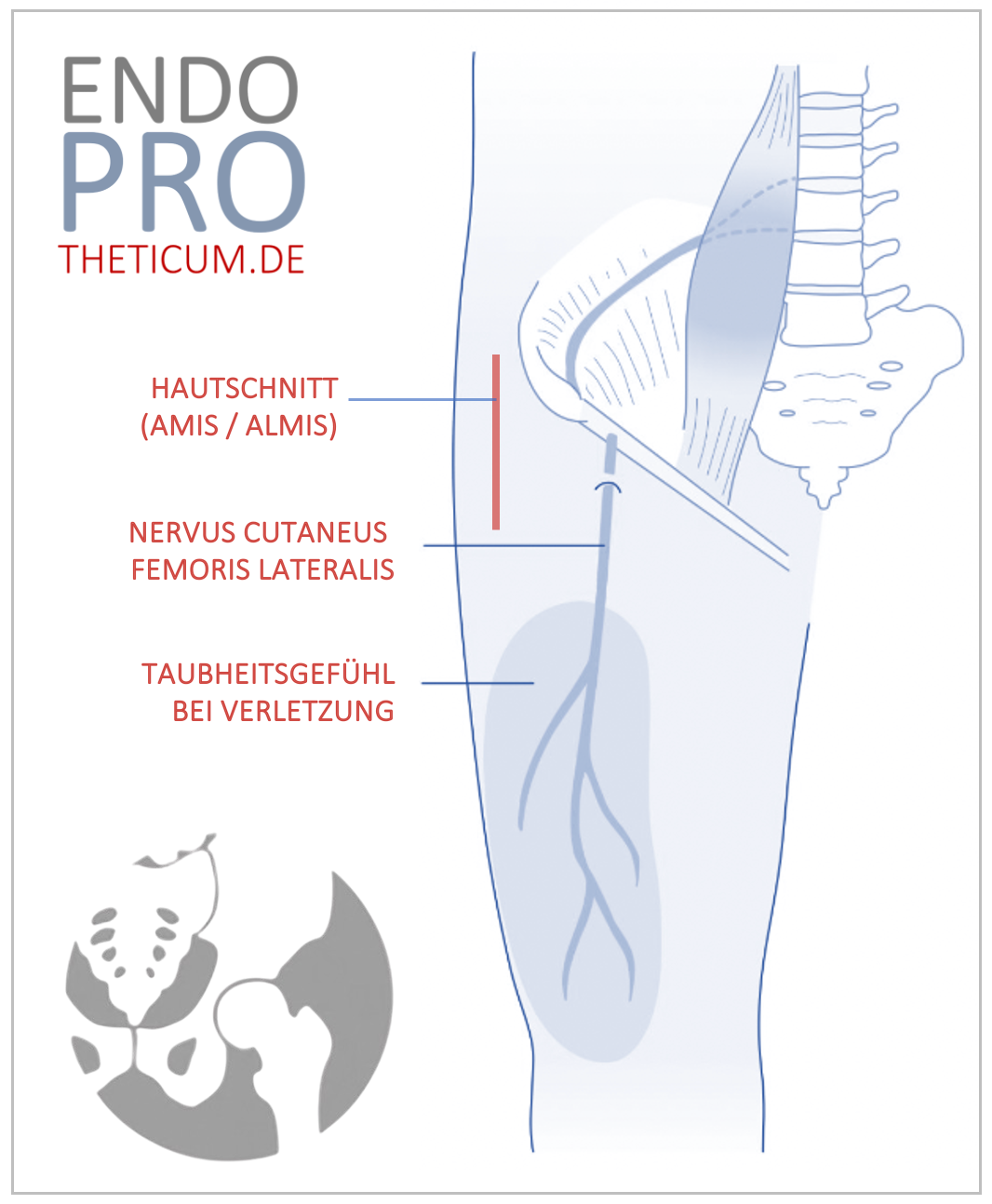
- Particular attention must be paid to possible nerve irritations when accessing via the anterior or anterolateral approach, as local hypersensitivity can occur.
Long-term effects
The combination of lymphatic drainage with light exercise therapy has shown in studies that patients are often mobilized more quickly after a total hip replacement and can move more often without pain in the long term. Satisfaction with the healing process was also significantly higher compared to therapy alone without lymphatic drainage.
Role of lymphatic drainage in modern rehabilitation medicine
The importance of manual lymphatic drainage (MLD) in postoperative therapy has increased significantly in recent years. Their integration into the overall rehabilitation concept shows clear advantages for the recovery process after joint replacement.
Holistic approach
Rehabilitation after joint replacement requires a multidisciplinary approach. Lymphatic drainage is increasingly being combined with other methods, such as:
- physical therapy
- Movement therapy
- Electrotherapy for muscle stimulation
- Nutritional advice
This integrative approach results in faster recovery times and lower complication rates.
Trust in modern medicine
Through the use of lymphatic drainage, patients experience an individually tailored therapy tailored to their well-being. This personalized approach promotes trust in modern medicine and therapeutic measures.
Long-term studies and future perspectives
Current studies show that the early use of lymphatic drainage in the postoperative setting improves the functionality of the joints in the long term. Innovative developments such as robot-assisted exercises combined with manual treatments will revolutionize the rehabilitation process in the future.
Practical tips for patients
Self-help to support lymph flow
- Exercise: Regular, light exercises such as tension exercises and walking.
- Compression: Wearing compression stockings to support the lymphatic system.
- Diet: Drink plenty of fluids and eat a balanced, anti-inflammatory diet.
Take warning signs seriously
If there is severe, persistent swelling or pain, patients should consult the surgeon if necessary.
Myths and frequently asked questions about lymphatic drainage
Myth 1: Lymphatic drainage is painful
- Correction: Lymphatic drainage is gentle and relaxing. Pain is a sign of improper execution.
Myth 2: Swelling goes away without treatment
- Correction: Although slight swelling can go away on its own, targeted treatment speeds up the process significantly.
Frequent question: Is lymphatic drainage necessary with every joint replacement?
- The decision depends on the individual healing process, but is very helpful in most cases.
Conclusion - lymphatic drainage after joint replacement is extremely important!
Manual lymphatic drainage is more than just a supportive measure - it is a fundamental component in the rehabilitation process after the use of a knee or hip prosthesis. Their ability to efficiently reduce swelling and promote the circulation of lymph not only accelerates the healing process, but also significantly increases patient comfort.
Patients often report a faster recovery of their mobility and improved freedom of movement. Lymphatic drainage also offers the great advantage of supporting the healing process non-invasively and gently.
Lymphatic drainage plays a crucial role, especially in the early postoperative phase, in preventing risks such as edema or secondary complaints due to fluid accumulation. Their effectiveness is enhanced by their precise technique, which is adapted to the lymph flow, and the close collaboration with other forms of therapy such as physiotherapy.
Despite its many advantages, manual lymphatic drainage often remains an underestimated aspect of aftercare. In times of staff shortages, this personnel-intensive form of therapy is now offered too rarely.
Anyone who actively takes part in relieving and healing measures such as manual lymphatic drainage after a joint replacement is actively investing in their recovery and long-term quality of life. Expert care and regular sessions can help you take full advantage of the positive effects of lymphatic drainage - a further step towards a pain-free, active life with a new prosthesis.
Armed with this knowledge, manual lymphatic drainage should not be missing from any therapy plan as part of a comprehensive rehabilitation strategy after a knee or hip prosthesis.
MAKE AN APPOINTMENT?
You are welcome to make an appointment either by phone or online .